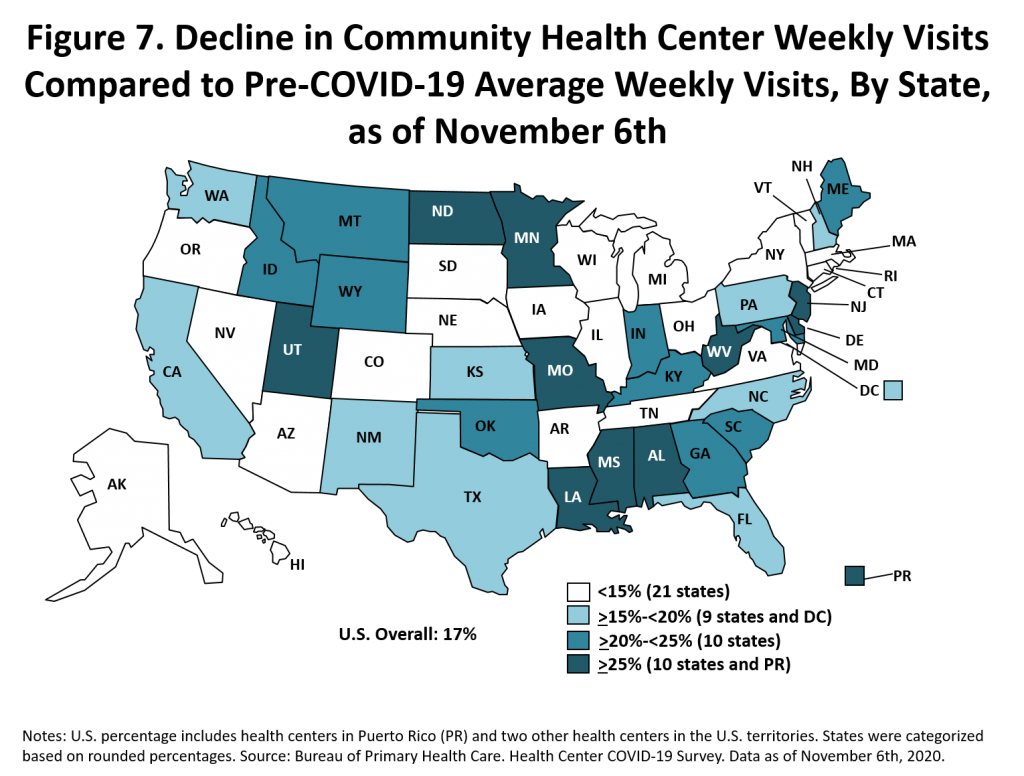
As the nation entered the worst phase of the COVID-19 pandemic to date, our latest data note updates previous findings on the impact of COVID-19 on community health centers. The data note is based on survey data collected by HRSA, as reported for the week of November 6, 2020, and also reports updated trends data for the seven-month period from April 3 through November 6.
Community health centers have tested 5,035,426 patients for COVID-19 virus over seven months, since reporting began in April. The number of patients tested for the COVID-19 virus this week (244,945) neared the peak level (251,246) reported in mid-August. In the aggregate, a total of 561,777 health center patients have tested positive for the COVID-19 virus, accounting for 5.8 percent of cases nationally, or one in 17 of all U.S. cases. Patients reported as racial and ethnic minorities, particularly Hispanic/Latino patients, accounted disproportionately for those who tested positive, both this week and consistently over the seven months of survey data. While CHC operational capacity has improved, weekly visits remain consistently lower than before the pandemic. With no additional federal COVID-19 financial relief committed, the pandemic has taken an enormous financial toll on health centers, resulting in an estimated $3.714 billion in cumulative patient revenue losses over seven months. In the face of deep financial loss and continued uncertainty, the future of our nation’s health centers should be a cause for both deep concern and renewed long-term support.
The data note was produced by the Geiger Gibson/RCHN Community Health Foundation Research Collaborative.
Read the date note, “Key Updates from the Health Center COVID-19 Survey (Week #32): The Status of Community Health Centers as the Nation Enters the Worst Phase of the COVID-19 Pandemic”
__________________________________________________________________________________________________________________________
Community Health Center Telehealth Utilization in Rural and Urban States During the COVID-19 Pandemic
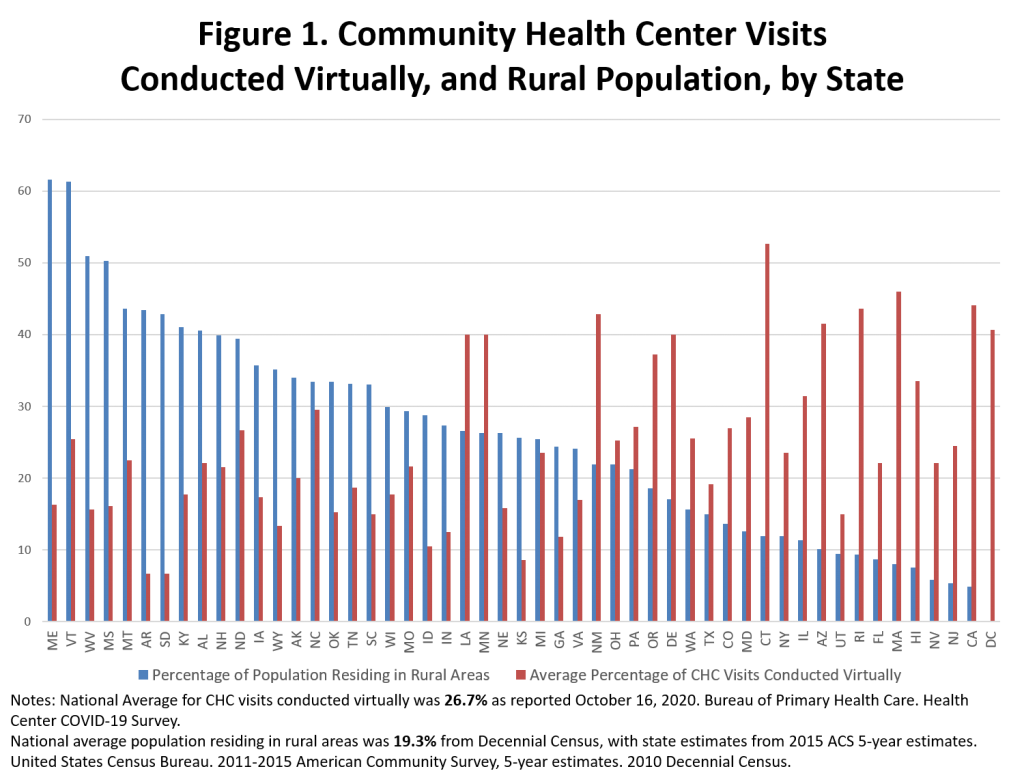
In the wake of the COVID-19 pandemic, many community health centers rapidly pivoted to providing telehealth and virtual visits. A recent analysis by the Geiger Gibson/RCHN Community Health Foundation Research Collaborative at the George Washington University’s Milken Institute School of Public Health reports on community health center telehealth utilization in urban and rural states during the COVID-19 pandemic.
Analyzing data from HRSA’s weekly COVID-19 survey, researchers document that during the peak of health center telehealth utilization, which occurred the week of April 24th, 54 percent of community health center visits, on average, were conducted virtually. This percentage had fallen by half as of October 16th, with virtual visits accounting for just over a quarter of visits that week. States with a higher percentage of the population residing in rural areas tended to have a lower proportion of health center visits conducted virtually. Among those were more-rural states in the Midwest census region (KS,NE,SD,) as well as and the West (ID, UT and WY) and the South (AR, GA, SC, OK, WV) regions. States with less-rural populations located in the Northeast (CT, DC, DE, MA, RI) and West (AZ, CA, HI, NM, OR) reported a higher percentage of telehealth utilization than their rural counterparts.
While telehealth utilization appears to be widespread, there may be important differences in the availability of services by location, with health centers in more-rural states less likely to offer virtual visits. Barriers and challenges to expanding telehealth, including payment parity, cost, and the availability of robust infrastructure, should be the focus of analysis as well as policies to improve access to care in all communities.
Read the data note, “Key Updates from the Health Center COVID-19 Survey (Week #29): Community Health Center Telehealth Utilization in Rural and Urban States During the COVID-19 Pandemic”
__________________________________________________________________________________________________________________________
Health Policy in the New Administration: A Geiger Gibson Webinar Series
Please join us for a special webinar series hosted by the Geiger Gibson Program in Community Health Policy starting January 21st, 2021. Registration is open through January 19th.
This four-part series will cover key federal health policy issues especially important to community health centers, health center networks, and state and regional primary care associations:
- The Biden administration’s blueprint for action – what does it mean for health centers and their communities?
- Insuring all low-income people – where is the administration headed?
- How will reducing health disparities guide administration policymaking?
- Health policy and immigrant health.
The series will be hosted by Sara Rosenbaum, J.D., Harold and Jane Hirsh Professor of Health Law and Policy, the Milken Institute School of Public Health at The George Washington University, and will feature presentations by leading experts from the University and the broader Washington, D.C. policy community.
Webinar program information including dates, fees and registration can be found here.
__________________________________________________________________________________________________________________________
5th Annual John W. Hatch Lecture – Health Equity at Scale
The FaithHealth Division of Wake Forest Baptist Health and Shaw University Divinity School is hosting the Fifth Annual John W. Hatch FaithHealth Lecture Series. This year’s event, themed Health Equity at Scale, will take place on Tuesday December 1, 2020, 10 am – 3:30 pm EST.
The Series is named in commemoration of the pioneering work of Dr. John W. Hatch, William Rand Kenan Jr. Professor Emeritus, Health Behavior and Health Education, University of North Carolina Gillings School of Global Public Health. Dr. Hatch, who helped launch the nation’s first rural health center in Mound Bayou, Mississippi, has had an extraordinary career of more than fifty years, focusing on the areas of faith, health, and community organization with a special emphasis on underserved communities and social justice.
Keynote speakers include Dr. Somava Saha, Executive Lead for Wellbeing In the Nation (WIN) Network; Founder and Executive Lead for Well-being and Equity (WE) in the World; Founder and Executive Lead for 100 Million Healthier Lives, and Richard “Stick” Williams i the former Vice President of Corporate Community Affairs at Duke Energy Corporation and President of the Duke Energy Foundation. Dr. John W. Hatch and E. Benjamin Money, MPH, Deputy Secretary for Health Services-N.C. Department of Health and Human Services, will also participate in the program.
This is a free event, but pre-registration is required. For more information and to register, visit FaithHealthNC’s website: https://faithhealthnc.org/hatch-faithhealth-lecture-5/
__________________________________________________________________________________________________________________________
ICYMI: Months into the COVID-19 Pandemic, Community Health Centers Report Signs of Improvement, But Face Financial Uncertainty.

__________________________________________________________________________________________________________________________
We wish all of our colleagues and friends a happy Thanksgiving. This season especially, we give thanks to the migrant and seasonal agricultural workers whose labor ensures that we have access to food throughout the year, and to the community health centers that have demonstrated a long-standing commitment to the health and well-being of agricultural workers.
Earlier this year, we reached out to our colleagues at Finger Lakes Community Health (Penn Yan, New York) and Oak Orchard Health Center (Brockport, New York) and to the National Center for Farmworker Health, Inc. (NCFH) to learn more about the impact of COVID-19 on agricultural workers, who have been essential workers, toiling in fields, farms and orchards amidst a global pandemic. Enjoy the holiday, stay safe and well – and join us in recognizing America’s agricultural workers!
Read “Amidst a Pandemic, Agricultural Workers Toil and Community Health Centers Adapt and Innovate”

Apple Harvest. Photo via Maine Mobile Health Program. Learn more on their chcCHroniCles profile



