Advancing and Promoting Community Health: Opportunities for Accountable Communities for Health and Community Health Centers
A new issue brief examines community health center engagement within Accountable Communities for Health (ACHs) and identifies opportunities and challenges for CHC participation. ACHs are multi-sector, community-based partnerships that aim to address community health and social needs. They share much in common with community health centers – local, non-profit community-governed health care providers which by mission and mandate offer comprehensive primary and preventive care to underserved populations and high-need communities. Both ACHs and CHCs play a critical role in addressing health-related social needs and social determinants of health.
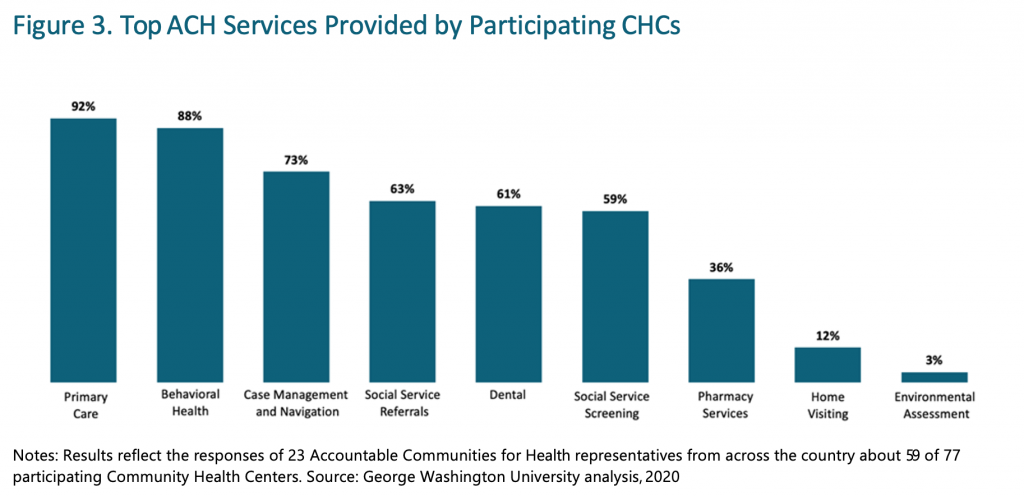
Our colleagues at the Funder’s Forum on Accountable Communities conducted a survey of ACHs about CHC participation and engagement, and follow-up conversations with ACH and CHC representatives. They found that ACHs frequently partner with CHCs, and CHCs often participate in the governance of ACHs. Participating CHCs typically provide a number of services and have leading or supporting roles in various programs, most often related to reaching underserved populations, assessing community health needs, serving as a resource/linkage to other human services, and building community engagement and trust. However, strengthened CHC capacity, staffing, and funding, as well as technology for data sharing, are needed in order to achieve active and broader CHC participation in ACHs.
The researchers suggest that federal policy makers provide opportunities for stronger relationship-building between CHCs and other key stakeholders that may participate in an ACH, give those CHCs that participate in an ACH more flexibility in how they spend their federal grants, explore support for CHCs as AHC backbone organizations, encourage CHC engagement in ACH initiatives through Alternative Payment Methodology incentives, and standardize approaches to data systems and data collections. These steps are essential as community health centers and safety-net providers seek to recover from the devastating impact of the COVID-19 pandemic on their operations and communities.
The brief was produced by The Funders Forum on Accountable Health and Geiger Gibson/RCHN Community Health Foundation Research Collaborative.
Read the issue brief.
__________________________________________________________________________________________________________________________
In Tribute to Dr. H. Jack Geiger
In the final days of 2020, the community health center movement lost a legend, the inimitable Dr. H. Jack Geiger, who has inspired all of us who have worked in and with health centers the world over. It was Dr. Geiger’s commitment to health care justice and lifting people out of poverty that launched the community health center movement in the U.S. In June 1965, the Office of Economic Opportunity (OEO) awarded a grant for the establishment, as a research and demonstration project under the sponsorship of Tufts University, of the nation’s first two health centers. The health centers, a response to widespread urban and rural poverty and striking racial and income disparities in health outcomes, were conceived by Dr. Geiger after his experiences working with community health pioneers Drs. Sidney and Emily Kark in Pholela, South Africa, and spending time in the Delta during the “freedom summer” project of 1964, a volunteer campaign to register African American voters in Mississippi.
With the support of Dr. Count Gibson, the head of Tuft’s Department of Preventive Medicine, Dr. Geiger proposed a care delivery model based on the Kark’s principles of Community Oriented Primary Care (COPC), a model of care that integrates primary care medicine with population-focused public health.
The urban site in Columbia Point (MA) opened in December 1965, and search for a rural, southern site began in earnest that same year, leading to the selection of Mound Bayou, the oldest predominantly Black community in America. Dr. Geiger, who served as the project director for both the Boston and Mound Bayou community health centers, arrived in Mound Bayou in 1966. Dr. John W. Hatch, the Center’s Director of Community Health Action, came later that year to begin the community organizing and outreach work of the Tufts Comprehensive Community Health Action Program, of which the health center was a part. After nearly three years of planning, the Tufts-Delta Health Center opened its doors in November 1967 in a rented five-room church parsonage at the Lampton Street Church of Christ in Mound Bayou, a testament to Dr. Geiger’s deep commitment to equity, his pioneering spirit and his collaboration with an extraordinary project team. We had the great pleasure of recording Dr Geiger, in conversation with Dr. Hatch, and hearing his reflections on health, health care, and the founding of what ultimately became a health center program that today serves 30 million people across the U.S. You can view the first of our 5-part video series here, Part 1: Dr. H Jack Geiger and Dr. John Hatch on the Earliest CHCs.
Ever committed to bettering the world, Dr. Geiger’s work extended beyond the health center movement. With like-minded colleagues, he co-founded Physicians for Social Responsibility and later, Physicians for Human Rights. A trailblazing advocate, Dr. Gieger was a teacher and mentor of the first order to decades of students, first at Tufts University School of Medicine, then at the School of Medicine of the State University of New York at Stony Brook, and finally at the City University of New York Medical School, where he continued until his retirement as the Arthur C. Logan Professor of Community Medicine.
Dr. Geiger’s profound vision, unwavering commitment to equity, and deep engagement in the struggles for human rights, civil rights and health care justice are unparalleled. He has left us an extraordinary legacy – and we will continue the fight for health equity, in his name. May his memory be for a blessing, and for a revolution.

Dr. H. Jack Geiger was the keynote speaker and honored guest at our book launch for “Out in the Rural: A Mississippi Health Center and its War on Poverty” by Dr. Thomas J. Ward, Jr. which details the founding of the Tufts-Delta Health Center in Mound Bayou, MS. (2016)
Find more about the book “Out in the Rural: A Mississippi Health Center and its War on Poverty”
View photo gallery.
__________________________________________________________________________________________________________________________
The New, Adapted and Improved Geiger Gibson Fellowship in Community Health Policy
Calling all health center, PCA and HCCN staff: Are you interested in taking a deep dive – from the comfort of your own workplace or home – to learn more about health policy and how to advocate for health center needs? Do you want to gain or hone skills to make you more effective in your job, or to help advance your career?
The Fellowship program is designed to help mid-level and senior health center, PCA, and HCCN staff develop a deeper understanding of health policy and advocacy. It provides rising leaders in the health center movement with an immersive experience in federal health policy, and assists participants in developing basic health policy analysis competencies so that they can engage effectively in advocacy.
What’s new?
- We have re-worked the Geiger Gibson Fellowship in Health Policy to address the current reality of the COVID pandemic and challenges with travel.
- All sessions will take place over Zoom instead of in-person.
- Instead of an intensive multi-day trip to DC, the Fellowship will consist of 20 sessions, each about 1.5 hours long, running from March 2021 through December of 2021 – typically on Wednesdays from 12:00 to 1:30 pm eastern time.
(We will publish a full schedule once we have all dates and speakers lined up, but we expect sessions to be held about 2 times a month, give or take a few…) - We have reduced the cost from our in-person Fellowship down to $750 per person.
What’s the same?
- We will still provide the same high-quality content as we have in years past.
- We will still include access to health policy experts, leaders in federal agencies, Capitol Hill staff, and peer networking opportunities.Program faculty include senior NACHC staff, faculty at Milken Institute School of Public Health, Washington DC-based health policy experts, Geiger Gibson Distinguished Visitors, leaders in federal agencies and Capitol Hill staff.
- We will still have a mix of policy content skill-building learning sessions.
- We will still be hosted by Zoë Beckerman, Sara Rosenbaum, and Feygele Jacobs.
- And we will still include small-group work to problem solve and develop sample advocacy materials, and the opportunity for a mock Hill visit and critique of your approach.
The first two sessions will be held on the following dates:
- Session 1: Wednesday March 17, 2021 from 12-1:30 pm eastern time.
- Session 2: Wednesday March 31, 2021 from 12-1:30 pm eastern time.
Additional sessions will be scheduled very soon, with dates running from April through December.
For any content or eligibility questions, please contact Zoë Beckerman at jzbecker@gwu.edu
Cost: Participation in the Geiger Gibson Health Policy Fellows Program costs $750
More info: https://publichealth.gwu.edu/projects/geiger-gibson-program-community-health-policy#healthpolicyfellowsprogram
Application form: https://publichealth.gwu.edu/content/geiger-gibson-program-health-policy-fellows-application-form
__________________________________________________________________________________________________________________________
Our Impact
For many of us, the beginning of a new year is a good time to take stock of what we’ve accomplished, where we may have fallen short, and plan for what’s next. Since our founding in 2005, the RCHN Community Health Foundation has developed a wide range of projects and collaborated with community health centers, primary care associations, and public health institutions across the country to support community health centers and improve access to health care for the communities they serve. Our work encompasses direct grant making and community investment, technical assistance in support of health center capacity building and transformation, and a unique academic and research partnership with the Geiger Gibson program at GW’s Milken Institute School of Public Health. “By the Numbers” showcases the impact and reach of our diverse work as the nation’s only foundation dedicated to advancing the community health center movement. We are so proud to work with all of you to make this possible.




